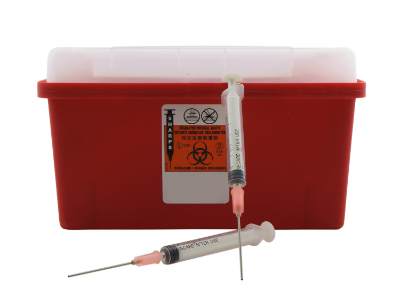
Training in fire safety is not only required by the major regulatory agencies; it is common sense. Any health professional who has lived through a fire in a care setting knows and has night terrors about the complexity of moving ill clients out of harm’s way in an emergency.
OSHA, the Occupational Safety and Health Administration, and NFPA, the National Fire Protection Association, both have strong guidance on healthcare facility safety. Point of trivia: when CMS surveyors investigate an organization’s physical safety and disaster planning, they pull out the NFPA guidelines and go by them. To satisfy CMS, know, follow, and exceed NFPA guidelines.
| Agency Regulation | Annual Required Training |
|---|
| TJC EC.02.03.03 | Annual Fire Drill Training |
| OSHA 1910.156(c)(2) | Annual Fire Brigade Training |
| OSHA 1910.157(g)(2,4) | Annual Portable Fire Extinguisher Training |
| OSHA 1910.158(b)(10) | Annual Fixed Fire Extinguisher Training |
(JCR Staff, 2024h; N.C. Department of Labor, 2022)
In healthcare, we are all expected to render assistance during situations that place our clients at risk. We, therefore, all require a working understanding of fire response, small fire suppression, and tactics to slow the spread of larger fires. As found in OSHA regulations, a fire brigade designation does not pertain to every health worker but to those who have received additional fire suppression and rescue instruction. If you have the floor or unit staff designated as “safety officers” or “fire wardens,” please review the OSHA Fire Brigade definitions to ensure they receive correct training before an inspection or cross your fingers before you are called to perform in an emergency.
| Agency Regulation | Ongoing Required Training |
|---|
| TJC EC.02.02.03 | Quarterly unannounced fire drills, all shifts, varying conditions, with staff participation. |
NFPA 16.14.3.10.2
NFPA 16.14.3.10.3 | Continuing safety education and supervision shall be provided for Operating Room staff (and others), incidents shall be reviewed monthly, and procedures shall be reviewed annually.
Fire exit drills shall be conducted annually or more frequently as the applicable code determines. |
(JCR Staff, 2024e; NFPA, n.d.)
For all of us, when you enter a new work area, look around and find fire alarms, fire extinguishers, exit signs, and oxygen cut-off valves. One way to remember fire safety is the acronym RACE.
- R: rescue
- A: alarm
- C: contain the fire (if possible)
- E: extinguish or evacuate
Never hesitate to sound the alarm with any suspicion of fire, yet never “fire.” Yelling “fire” creates panic. Instead, call out the facility's verbal code for fire. Call the switchboard to report the fire and pull the fire alarm. When you call the switchboard, please stay on the phone long enough to ensure they have received the correct information, such as where you are!
If a fire is small and confined, you may be able to extinguish it. If a client’s garments are on fire, wrap them tightly in a large blanket to extinguish the flames. If a piece of equipment catches fire, pull the plug or cut the electricity as soon as possible.
OSHA is clear if you place hand-held portable fire extinguishers for staff to use in emergencies, you must train every staff member annually on how to use them. Portable fire extinguishers come in different classes for use on fires of diverse sources. The extinguisher has small pictures on the label that help you identify the type of fire source material they should be used on. Class A puts out fires involving ordinary combustibles. Class B extinguishers smother fires involving flammable liquids or gases. Class C extinguishers put out fires in or near electrical equipment. Type ABC extinguishers can be used to fight all three types of fires.
To use an extinguisher, remember PASS:
- Pull the pin
- Aim the nozzle at the base of the fire
- Squeeze the trigger while making
- Sweeping strokes with the extinguisher plume
If a fire cannot be extinguished and smoke, fumes, or flames threaten client safety, you may need to evacuate. Evacuate ambulatory clients first. Stay calm and give clear directions. Evacuate horizontally for as long as you can. Then, evaluate vertically down to a lower level. Never use an elevator to escape during a fire. A sudden loss of power could leave you and your client trapped inside the elevator.
Healthcare units are required to be separated by heavy fire doors that close automatically when the alarm is sounded to keep the fire from spreading. To confine a fire, close the doors, windows, and all vertical openings like the laundry chute. Stuff wet towels under the doors to keep smoke out. Shut off oxygen supplies if directed to do so. Usually, facility policy designates someone in supervision to decide when to turn off oxygen supplies.
When rescuing anyone in immediate danger, remember to stay low. Smoke rises to the ceiling, forming a heavy, dense cloud that slowly descends. This cloud is deadly because it contains toxic gases.
Staff responsible for inspecting, maintaining, or repairing fixed fire extinguishing equipment such as sprinklers or fire hose reels must be trained annually concerning these essential safety items.