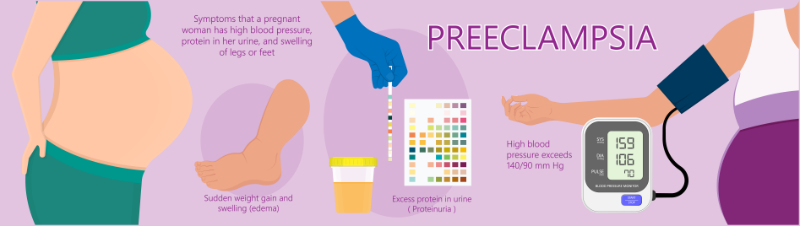
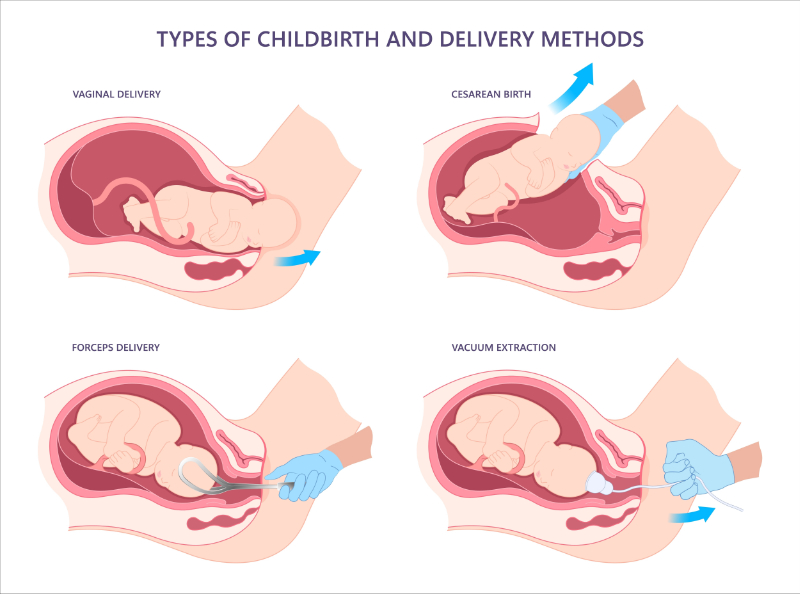
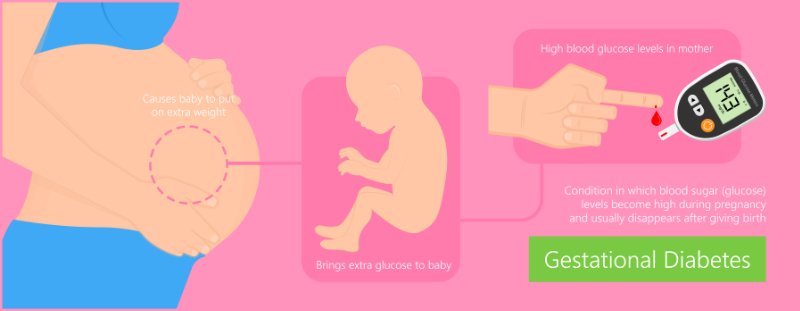
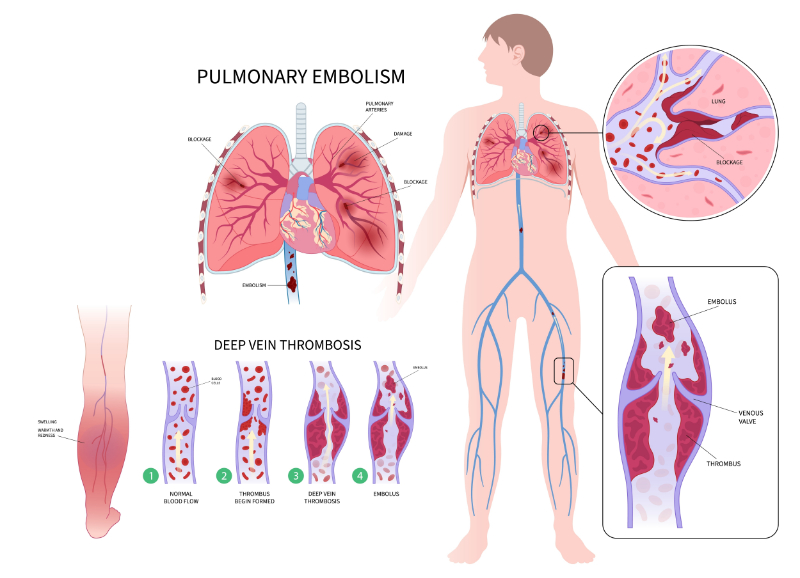
≥ 92% of participants will know how obesity can impact pregnancy.

Popular Courses
- Annual Regulatory Requirements, Current Practice
- Controlled Substance Prescribing: The Tennessee Chronic Pain Guidelines
- Ohio Law Governing Drugs and Prescriptive Therapy
- HIV/AIDS: Current Evidence-Based Practice (Two Hour)
- Child Abuse: Pennsylvania Mandated Reporter Training, 3 hours - Initial Licensure
- Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with COVID-19
- Domestic Violence, Sexual Violence, Intimate Partner Violence
- Long-term Care Nursing: Admission and Medicare Documentation
- Alzheimer's, Dementia, and Related Issues