The role of the clinician working with an ostomy patient is that of an educator. The first encounter with a patient with an ostomy is critical, and when it takes place, it is equally important. For a patient who is preparing for surgery that will result in the creation of an ostomy, the clinician should preferably meet with the patient weeks or days prior to surgery. An optimum time would be during one or more visits to the provider's office; this is an opportunity to give a broad overview of what an ostomy is, allowing the patient to see and handle ostomy supplies, such as a pouch, clip, and wafer. During this time, providers should address questions from the patient, significant other, or family. Arranging for the patient to meet with an 'ostomy visitor' who has successfully gone through similar surgery can help lessen the patient's anxiety and provide reassurance. Permission from the patient must be obtained before arranging such a visit.
One thing the clinician must keep in mind is that the ostomy is probably not the patient's main concern. Their attention is focused on the disease or malfunction that necessitates surgery. The clinician can begin to gauge the patient's understanding of an ostomy by asking them what their surgeon has told them. The clinician should confirm this with the surgeon for a patient who is adamant that this will be a temporary ostomy and they don't need to spend time learning about it. If there is a possibility that the ostomy may end up being permanent, then it is important that the surgeon clarifies this with the patient.
Another scenario is a patient who ends up in the emergency department with severe abdominal pain or a traumatic injury, goes to surgery and wakes up with an ostomy. In these cases, there is no time for education or emotional preparation. These patients are often overwhelmed by the sudden change in their lives. They are grappling with what has happened and are not emotionally ready to learn about ostomy care.
The clinician must familiarize themselves with the case history and get input from the nursing staff caring for the patient and, if possible, the primary care provider and surgeon before interviewing the patient. Another important resource person is the social worker or case manager. They can advise the clinician about the patient's discharge plans and ask if there are concerns about the discharge. Does the patient need to go to a short-term rehabilitation center or skilled nursing unit before going home? The clinician will also need to ask about whether the patient's home environment is conducive to recuperation and ostomy care. This author encountered a patient in a clinic who had been discharged from another facility to a trailer home where the utilities and electricity had been cut off. In this care, the clinician and social worker must work together to review the patient's medical insurance coverage and sources for ostomy supplies. It is the patient's choice where to obtain ostomy supplies from. However, patients who have had no preparation for ostomy creation will need a great deal of help and guidance from the clinical and social worker with this step.
It is essential that patients going home with an ostomy have home healthcare. The patient may be resistant to having a 'stranger coming into my home.' It may appear as another step in losing control of their lives. The clinician needs to validate the patient's feelings and explain that home healthcare will help them regain their independence more quickly. Frequently, a patient will say, "My wife/husband/ partner will take care of it." This can be an assumption on the part of the patient without consulting their spouse or partner. The spouse or partner may or may not be willing to take on ostomy care. They may feel resentful, overwhelmed, or anxious about what is also a sudden change in their lives. A spouse or partner willing to become the caregiver will need ostomy education and training; the clinician can point out this to the patient, and the spouse or partner can reinforce this.
Hospital stays are short, and the clinician in the facility will have a very short window of time to work with the patient with a new ostomy. To maximize this time, priorities need to be set. The issues discussed above about preparing for discharge all need to be taken care of. The clinician may have the urge to cram in as much ostomy education as possible, "please read this, watch this, tell me any questions you have." However, this approach rarely works unless the patient is highly motivated to learn. The clinician's first meeting with the patient should focus on getting to know the patient, putting them at ease, and asking if they have any questions. The first meeting may often seem to be unproductive; the patient may have little to say, be withdrawn, resentful, or angry. The clinician can leave educational materials with the patient and suggest that if the patient feels up to it, they should look through them before their next visit.
The next important step while the patient is in the facility is for the clinician to change the ostomy pouch; this allows the clinician to inspect the stoma, to ensure that it is functioning properly, to observe the condition of the peristomal skin area, and to determine if the ostomy pouch being used is the best choice, given the characteristics of the stoma. Determine if the patient has a partner or caregiver willing to be involved in ostomy care, even if only as an observer, and if possible, have them present when the clinician does the first pouch change.
Perhaps the most important advice to give a patient with a new ostomy is that ostomy care is not difficult. They may not believe you at first, but if you can relate ostomy care to something in the patient's life, this is a good place to start. What was, or is, the patient's occupation and hobbies? Someone whose occupation requires using their hands, such as precision and accuracy with measurements or numbers, has transferable skills that can assist with ostomy care. One key component of care is sizing the stoma size and adjusting the wafer opening as needed. A patient or caretaker who sews will also have skills that can be employed in ostomy care.
The clinician should allow plenty of time for the first pouch change and talk through the steps with the patient and caretaker, if present, in an unhurried manner. Gather the supplies to complete the procedure, which includes washcloths or disposable wipes for cleaning towels for drying around the stoma. A receptacle, usually a bedpan, is used to empty the pouch before removing it. Usually, for this first pouch change, the patient will be in bed, but when they are up and about at home, they can empty the pouch directly into the toilet. A good tip to share with the patient and caretaker is to put a layer of toilet paper in the toilet before emptying to prevent splashing.
The clinician should demonstrate removing the clip from the end of the pouch, unfolding it, and emptying it; this is the most essential step that the patient must be able to do before going home. Once the new pouch is applied, the clinician will demonstrate how to apply the clip and then have the patient or caretaker do a return demonstration. Once the clinician has taught the patient how to empty the pouch, the clinician needs to reinforce with the nursing staff on the unit that the patient is able to empty their pouch with standby assistance from staff. These opportunities for the patient to practice emptying the pouch before discharge are critical. The clinician should follow up with the nursing staff to ensure this is happening and get feedback from the staff on any problems or concerns the patient has. It is not uncommon for the patient to tell the nurses that they have been taught how to empty the pouch, and once they are home, they will do it – but in the hospital, they want the nursing staff to do it.
The first home health care visit should occur the day after the patient is discharged. The first 24 hours at home can be very stressful for the patient. There is no call bell or nursing staff around to respond if they have a problem. As part of their discharge the facility clinician must ensure that the patient and family have a contact telephone number for the home health agency and when to expect their first visit. Although patients with new ostomies may not be discharged home either in the short term or long term, this course will focus on the care of the patient in the home setting since this is the most challenging, and many facets of the content are applicable to patients in other discharge settings, such as long-term care or assisted living.
The clinician's first visit to the patient at home should focus on the following primary goals, although others can be added at the clinician's discretion and as time permits.
The primary goal is for the clinician to establish a good rapport with the patient and significant other or caretaker. One of the best ways to achieve this is to listen closely to what the patient and significant other have to say, as well as their fears, concerns, and sometimes anger and frustration about the situation they find themselves in. The clinician may not have answers to many of these issues, but they can direct the patient to resources that may be able to provide more help, such as the case manager or social worker who works with the home health agency.
The next important goal is to establish the role of the home health clinician, which is that of an educator. It is important that the patient and family understand that the clinician is not there 'to do' the ostomy care but to teach self-care to the patient with the assistance of family or caretaker as needed. There is a limit to the number of home health visits set by the payer source, and it is critical to ensure that each visit is used as a step toward patient independence in ostomy care. The patient, significant others, and the clinician will develop a plan of care for the patient. This will include:
- The frequency of visits.
- What the patient and significant other will achieve at each visit.
- Troubleshooting any problems that may arise.
Another goal for the first visit is to determine the suitability of the patient's home environment for ostomy care and any modifications that might be needed. Depending on the clinician's background (nursing, physical therapy, or occupational therapy), they may have unique skills in evaluating a home setting. The patient may point out concerns they have, such as finding the toilet too low to sit on and empty the ostomy pouch. The clinician may recommend a raised toilet seat and explore with the patient and family ways of obtaining one.
With each home visit, the patient and family should learn another step in ostomy care until they can independently demonstrate emptying and changing the ostomy pouch.
The clinician should also review the patient's current medication profile. Problems with the absorption of medications can arise related to the type of ostomy created. For example, depending on the length of the small intestine removed, extended-release medications may not be absorbed at all or incompletely absorbed. The clinician needs to advise the patient and caretaker to discuss this with their pharmacist.
The important questions that the patient and caregiver will need answers to include:
- How often should the pouch be emptied?
- In one-piece drainable appliances, the pouch and wafer are permanently joined to each other, and they have an opening at the end of the pouch, which provides a way to drain the effluent from the end of the pouch whenever it gets 1/3 to 1/2 full. All ostomy pouches (colostomy, ileostomy, and urostomy) should be emptied when 1/3 to 1/2 full to prevent the weight of the pouch from pulling the wafer away from the skin. Because closed-end pouches are meant to be disposable, they are most often appropriate for colostomies, in which the pouch may only need to be changed once daily or every couple of days.
- Is stoma care going to be painful?
- No, there are no sensory nerve endings in the stoma, which means that the patient does not experience any sensation.
- How often should the stoma be assessed?
- The stoma and surrounding skin surfaces should be carefully assessed each time the pouching system is changed. Since the stoma has no sensory nerve endings, the patient may not be aware of whether the stoma becomes lacerated or injured. The patient and caretaker are advised that the best way to prevent injury to the stoma is by always using a gentle technique when doing ostomy care. The pouch is first emptied, and then the pouch and wafer are gently removed, starting at the top and slowly pulling it away from the skin. Measuring guides are used carefully. Don't force a measuring guide that is too small over the stoma. Ensure that the edges of the measuring guide are smooth. The stoma can be gently rubbed and cleaned with a moist washcloth. Cleaning of the peristomal area should also be done with a gentle touch (United Ostomy Association of America [UOAA], 2023).
- Should the patient or caretaker be concerned if the stoma is bleeding?
- The stoma may have slight bleeding when it is being cleaned, which is not a concern. A stoma requires a good blood supply to stay healthy. However, suppose the patient or caretaker notices that blood is coming from inside the stoma, which could be a sign of intestinal bleeding, or they see blood in the stool or ostomy pouch. In that case, they need to contact their healthcare provider or ostomy clinician immediately.
- Does the pouch need to be rinsed out every time it's emptied?
- No, the pouch does not need to be rinsed. However, this is a personal choice; some feel more comfortable rinsing the pouch. But this practice can weaken the adhesive seal.
- Is there going to be an odor from the pouch that people will be able to detect?
- No, there should be no odor. Ostomy pouches are made to be odor-proof. This means that the odor stays in the pouch. When the pouch is emptied the person emptying the pouch will detect a fecal odor. But this is the only time that it should be noticeable. If this is stressful for the person emptying the pouch, there are in-pouch deodorants and odor eliminators that can be used. Keeping the bottom edge of the pouch clean is also important in preventing an odor.
- Is it possible to prevent the pouch from ballooning up with gas?
- There are pouches made from charcoal that are available with gas filters. They allow gas to escape from the pouch while absorbing odor. However, these do not work as well when the stoma effluent is very liquid, which is standard with an ileostomy. Liquid stool can block the filter.
- What can be done to ensure that the pouching system is going to stick to the skin?
- The skin barrier wafers that hold the pouching system in place are pressure-sensitive. A good seal depends on the wafer making maximum contact with the skin surface. One intervention the patient can do to aid this process is to apply gentle pressure to allow the wafer adhesive to come in full contact with the skin contours. After applying the new pouching system, the patient folds both hands over the wafer while resting comfortably. It is not necessary to lie down after changing the pouch, but if possible, the patient should avoid getting up and becoming active immediately afterward; this will also help the pouch to adhere more securely (Carmel et al., 2021).
- If the pouch starts leaking around the wafer a day or two before it needs to be changed, is it okay to seal it with tape?
- No, once the pouch starts leaking, it needs to be changed. Adding tape may keep the pouching system in place, but the drainage leaking on the peristomal skin can cause severe excoriation.
- How does a healthy stoma look?
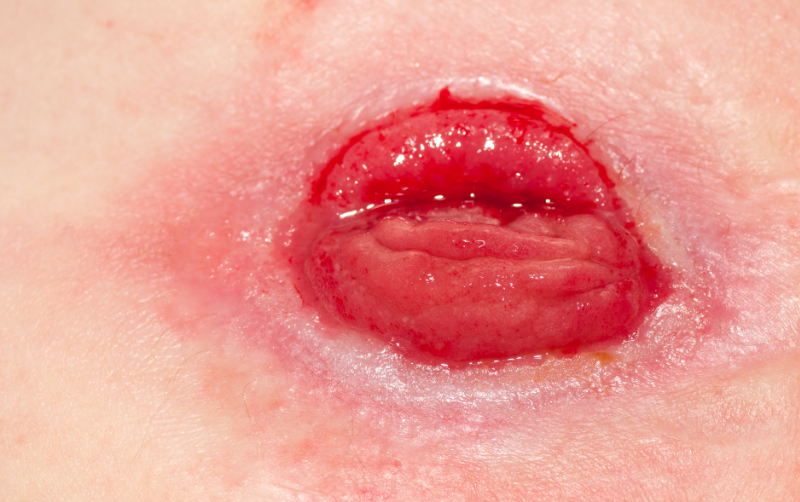
- Stomas should be "nicely budded," sitting about 1 ½ to 2 inches above skin level on the abdomen. However, this is a description of the 'idea' stoma; in real life, many stomas don't look like this. Stomas can be different, and challenges present at the time of surgery can result in stomas that are flat at skin level or retracted, which means they are below skin level. Despite their appearance, these are all functioning stomas. However, they can pose a challenge for pouching, which we will discuss further in the next section dealing with pouching appliances.
- Most stomas are a deep red color, apart from a ureterostomy, which is usually pale pink. The stoma should be moist and will be edematous in the immediate post-operative period. The edema will decrease gradually over the first 6-8 weeks after surgery (Carmel et al., 2021). As the edema resolves, the size of the stoma will change and become smaller. The os (opening of the stoma) should be nicely centered. However, in certain instances, this may not be the case. The clinician should ensure they can identify where the stoma opening is positioned and make the patient and caregiver aware of this. The stoma should be free of discoloration or growth.