Know Your Legal Rights as a Nurse
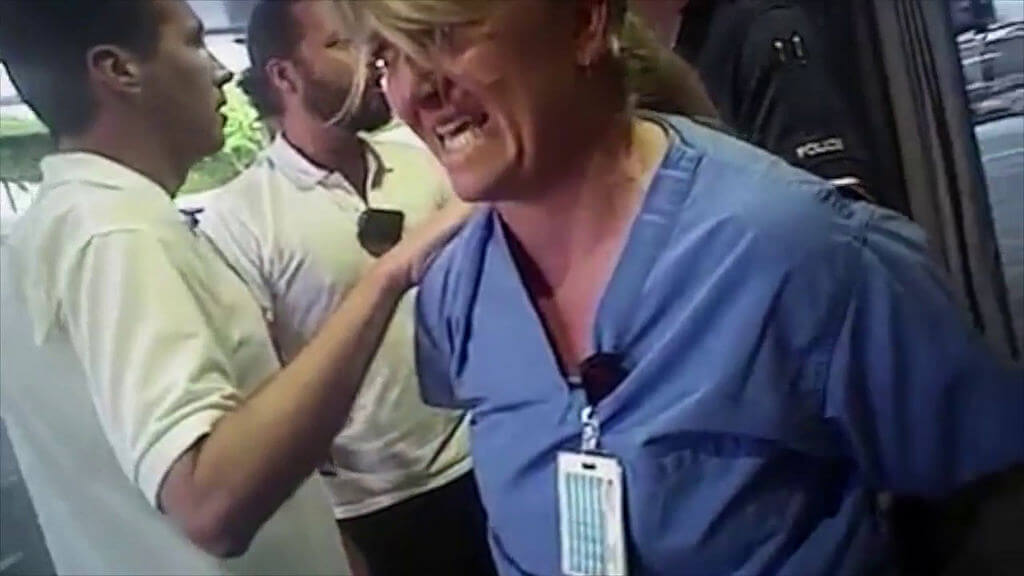
“I’m just trying to do what I’m supposed to do. That’s all.” Spoken by Utah nurse Alex Wubbels moments before she was arrested, these words echo a fundamental truth about nurses. Nurses are supposed to protect their patients, and the fact that nurses are the most trusted of all professionals indicates that they largely fulfill this duty.
But who’s protecting nurses? Nursing can be a dangerous job. For starters, nurses are at risk for violence. In fact, “in many states, being a nurse is more dangerous than being a police officer or a prison guard.” On top of that, “malpractice claims against nurses are increasing, with more than $90 million paid in nurses’ malpractice claims over a five-year period.”
In case you haven’t heard the Alex Wubbels story, here is the lowdown. Wubbels was the charge nurse in the University of Utah burn unit, which was caring for a patient who had just been in a car accident. The patient was not suspected of a crime, and he was unconscious. Detective Jeff Payne came in on July 26, 2017 and requested that Wubbels take a blood sample from the patient. Wubbels explained to the detective that there were three reasons she couldn’t get that blood sample for him: (1) the officer didn’t have a warrant, (2) the patient couldn’t give consent, and (3) the patient wasn’t under arrest. Payne then handcuffed Wubbels and placed her in an unmarked car, while Wubbels protested, “This is crazy.” She was released after approximately 20 minutes and was not charged with a crime, but the story quickly went viral, becoming a PR nightmare for everyone involved.
If you had been in Wubbels’ shoes, what would you have done? What could you have done?
Why are there laws regarding nursing?
Nursing requires specialized training, skills, and deep knowledge. As you know, it’s not easy to become or be a nurse. It’s a high-pressure, literally life-or-death job. Because of this, and “because nursing care poses a risk of harm to the public if practiced by professionals who are unprepared or incompetent, the state, through its police powers, is required to protect its citizens from harm. That protection is in the form of reasonable laws to regulate nursing.” In this way, patients are protected.
But again, what about protection for nurses? Legal protection for nurses specifically is relatively new. It wasn’t until 1975 that nurses were granted statutory protection for cases in which they might be sued because of their nursing practice. Before that, the profession of nursing wasn’t considered worthy of the protection granted other medical professionals.
As we mentioned, nurses are often put in the way of physical harm, but nurses can suffer in other ways, too. As a nurse, you may be sued for things like medication errors, falls, pressure ulcers and negligence. You might have to work in an unsafe environment, receive unfair financial compensation for your work and training, or be faced with ethical dilemmas that haunt you for years. The good news is that there are protections in place for these situations. Are you aware of them?
What are the laws regarding nursing?
Each state in the United States has a Nurse Practice Act (NPA), which in itself isn’t enough to guide nursing practice in the state. So each state has a board of nursing (BON) that develops administrative regulations to make the law more specific.
Each state’s NPA differs, so be sure to become familiar with the specific guidelines in your state. The National Council of State Boards of Nursing lists the NPAs as the following:
- Authority, power, and composition of a board of nursing
- Education program standards
- Standards and scope of nursing practice
- Types of titles and licenses
- Requirements for licensure
- Grounds for disciplinary action, other violations, and possible remedies
That last bullet and its “possible remedies” are what we’re focusing on here.
What are your rights?
As a nurse, you have at least seven of them. The American Nurses Association composed the Nurses’ Bill of Rights, listing “seven premises concerning workplace expectations and environments that nurses from across the United States recognize are necessary for sound professional nursing practice.”
While not a legal document, the Bill of Rights serves as a guide on how to achieve professional rights for nurses. You may be thinking to yourself, “What, exactly, is the point of a bill of rights if the law won’t back me up on them?” We’re here to show you how the law will back you up on each of these rights so that you can do your job fearlessly.
Right 1: Nurses have the right to practice in a manner that fulfills their obligations to society and to those who receive nursing care.
What are the issues?
We’ve experienced a lot of natural disasters lately. Because you’re a nurse, the news of all the suffering people undoubtedly tugged at your heartstrings, and you wanted to help. More importantly, the victims were in dire need of extra medical attention.
It’s not always a straightforward matter of volunteering. Licenses are area-specific. You can’t legally cross a border and start administering vaccines. Additionally, conditions during natural disasters are less than ideal, leaving patients at higher risk for infection and other problems. If a patient you administer to in a disaster gets worse rather than better, you may be left legally unprotected.
What laws have been enacted to protect nurses?
There need to be specific laws regarding nursing in disaster scenarios. Nurses must be assured of “legal protections such as liability standards, license verification, and definition of scope of practice for nurses and other licensed practitioners providing care in disasters.”
The Uniform Emergency Volunteer Health Practitioners Act (UEVHPA) is a model legislation that provides such protection. States that adopt this bill recognize the licensure of healthcare professionals during a declared emergency if those professionals have registered with an appropriate system. This measure “permits those professionals to enter the state and provide services without having to seek a license in the state where the emergency has been declared, greatly increasing access to care during a critically difficult situation where licensure boards may be swamped with requests or may be non-functioning due to the disaster.”
Since the model legislation was created in 2006, only 17 states have enacted it. But the American College of Surgeons is working to pass the UEVHPA in all 50 states and the District of Columbia.
Rights 2, 3, and 6: Environment
- Right 2: Nurses have the right to practice in environments that allow them to act in accordance with professional standards and legally authorized scopes of practice.
- Right 3: Nurses have the right to a work in an environment that supports and facilitates ethical practice, in accordance with the Code of Ethics for Nurses with Interpretive Statements.
- Right 6: Nurses have the right to a work environment that is safe for themselves and for their patients.
What are the issues?
"Work environment issues, such as nurse staffing, are linked with patient outcomes, length of stay, and chance of death,” according to the ANA.
Other work environment issues affecting rights 2, 3, and 6 include work schedules, levels of fatigue, disaster efforts, sexual harassment, and work culture. These issues affect everything from the quality of care for the patient to the quality of life for you as a nurse – which in turn affects the quality of care you can offer patients. Left to itself, a poor work environment can lead to a downward spiral.
What laws have been enacted to protect nurses?
Each state’s NPA has specific guidelines about providing professional, ethical, and safe workplace environments. For an example of such guidelines, here is a segment of Utah’s Nurse Practice Act Rule: Hospitals should “[promote] a safe and therapeutic environment by: (A) providing appropriate monitoring and surveillance of the care environment; (B) identifying unsafe care situations; and (C) correcting problems or referring problems to appropriate management level when needed.”
These guidelines provide direction for not only stopping poor environments from getting worse, but also for preventing poor environments in the first place. See your state’s NPA for more details.
Right 4: Nurses have the right to freely and openly advocate for themselves and their patients, without fear of retribution.
What are the issues?
This right takes us back to Alex Wubbels’ story, raising questions about patient consent, authority, and, of course, the duty of nurses to their patients. Wubbels certainly wasn’t the first nurse to face retribution for advocating for patients: Some other examples include a Veteran Affairs nurse who was demoted after reporting abuse of patients and a New Jersey nurse who was quarantined instead of permitted to return to work after testing negative for Ebola.
What laws have been enacted to protect nurses?
For reporting, federal and state laws require that nurses report to an appropriate agency when abuse has occurred against the elderly, children, or other vulnerable people. Make sure you follow these basic guidelines when reporting; they will protect you from potential liability down the road:
- “Have a ‘good faith belief’ or a ‘reasonable suspicion’ that an injury or injuries are the result of abuse or neglect.”
- Make the report confidentially so that your identity is not made public.
Unfortunately, there are no federal protections for employees who report unsafe or unethical situations, but some states have passed whistleblower legislation to protect those who do.
For patient consent, many medical procedures could be considered battery if performed without patient consent. With a patient’s consent, healthcare professionals have the right to give care without fear of prosecution.
For giving care in undesirable circumstances, the UEVHPA protects nurses who volunteer in emergency situations.
Right 5: Nurses have the right to fair compensation for their work, consistent with their knowledge, experience and professional responsibilities.
What is the issue?
Getting fair pay.
What laws have been enacted to protect workers?
There are not any laws defining what “fair pay” means, except that minimum wage is $7.25. So if you’re not making $7.25 an hour, you should probably complain.
Depending on your pay scale, you may be exempt from receiving overtime pay. But that’s only if you make $913 per week, which, according to the Department of Labor, you probably should. Professionals qualify for this pay scale (and overtime exemption) when they “primarily perform work that either requires advanced knowledge in a field of science or learning, usually obtained through a degree, or that requires invention, imagination, originality, or talent in a recognized field of artistic or creative endeavor.”
The ANA recommends that you become familiar with the market wages in your area so you can seek employment that offers competitive pay, or at least not low pay.
Right 7: Nurses have the right to negotiate the conditions of their employment, either as individuals or collectively, in all practice settings.
What are the issues?
To join a union or not to join a union—that is the issue. There are long lists of pros and cons to joining a nurses union, and union laws and practices vary from state to state. Decide for yourself based on the laws in your state if joining a union is right for you.
If you’re not part of a union, be sure you understand what to look for when negotiating an employment agreement.
What laws have been enacted to protect workers?
The National Labor Relations Act protects employees on both sides of the issue: You are protected from employers if you are a part of a union and you are protected from unions if you are not part of a union. The law forbids employers and labor unions from “interfering with, restraining, or coercing employees” in regards to unions.
What can you do to protect yourself?
There are laws in place to protect you from the dangerous world of nursing. Despite the great intentions of these laws, unfortunately, you may still end up getting roughed up along the way. Remember Wubbels, who was just doing what she was supposed to. Become your own safety net by following these three tips:
- Know your hospital’s policy. If you follow the policies, the hospital will be able to defend you through the legal process. If not, no such luck.
- Keep yourself physically safe. There’s no need to succumb to paranoia, but there are some simple things you can do to protect yourself at work.
- Follow standards of care vigilantly. In other words, be a responsible nurse. If you’re ever caught up in a malpractice suit, you will be judged partially on whether you gave reasonable care&md
Get All Your State Nursing CEUs for One Low Price of $39
As nurses, we all just want to do what’s right and care for patients the best way we know how. As you perform your nursing duties, knowing your rights and the laws surrounding them will keep you safe and allow you to continue your good work for years to come.